Introduction
Fibromyalgia is a chronic pain syndrome marked by widespread musculoskeletal pain, fatigue, and tenderness in specific areas of the body. It is a complex disorder involving abnormalities in central pain processing, leading to an increased sensitivity to pain stimuli. The condition is more common in women and often develops between the ages of 30 and 50. Although not life-threatening, it significantly affects physical function and quality of life.
Causes and Contributing Factors
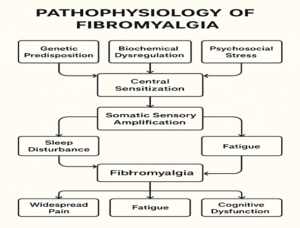
The exact cause of fibromyalgia remains uncertain; however, it is widely accepted as a multifactorial condition involving neurochemical, genetic, and environmental factors.
- Central Sensitization – Enhanced pain sensitivity results from changes in how the brain and spinal cord process pain signals, amplifying pain perception.
- Genetic Predisposition – Fibromyalgia often runs in families, suggesting a genetic component related to serotonin and dopamine regulation that affects stress and pain responses.
- Physical or Psychological Stressors – Physical trauma, infections, or emotional distress can trigger the onset or aggravation of symptoms in predisposed individuals.
- Sleep Disturbances – Non-restorative sleep and frequent awakenings disrupt hormonal balance and pain modulation mechanisms.
- Hormonal and Neurotransmitter Imbalance – Dysregulation of neurotransmitters such as serotonin, norepinephrine, and dopamine contributes to altered mood and pain perception.
Clinical Presentation
Patients with fibromyalgia often report a combination of chronic pain, fatigue, and cognitive complaints that interfere with daily activities. Common clinical features include:
- Widespread musculoskeletal pain
- Morning stiffness
- Fatigue
- Sleep disturbances
- Cognitive dysfunction (‘fibro fog’)
- Headaches and migraines
- Somatic symptoms such as IBS or TMJ pain
- Emotional disturbances like anxiety or depression
Diagnostic Criteria
The diagnosis of fibromyalgia is clinical, based on characteristic symptoms and the exclusion of other causes of chronic pain. Laboratory tests are typically normal and mainly used to rule out other disorders such as hypothyroidism, rheumatoid arthritis, or lupus.
American College of Rheumatology (ACR) Diagnostic Criteria (2010 / Updated 2016):
- Widespread Pain Index (WPI) and Symptom Severity Scale (SSS): WPI ≥ 7 and SSS ≥ 5, or WPI 3–6 and SSS ≥ 9.
- Duration of Symptoms: Symptoms must be present for at least three months.
- Exclusion of Other Disorders: The symptoms are not explained by another medical condition.
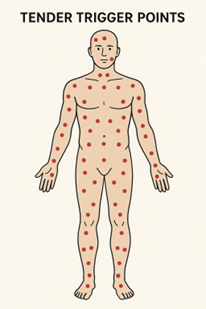
Tender Point Examination (1990 Criteria): Earlier guidelines identified fibromyalgia by widespread pain lasting more than three months and tenderness in at least 11 out of 18 specific tender points upon palpation.
Common Symptoms
Fibromyalgia involves multiple systems and produces both physical and psychological symptoms, including:
- Generalized pain and tenderness
- Persistent fatigue
- Sleep irregularities
- Cognitive dysfunction (‘fibro fog’)
- Sensitivity to temperature, light, and sound
- Digestive disturbances (IBS)
- Emotional distress or depression
Treatment Approaches
Fibromyalgia management focuses on symptom control through an individualized, multidisciplinary plan combining medication, exercise, psychological support, and lifestyle adjustments.
- Pharmacological Management – Includes analgesics, antidepressants (duloxetine, milnacipran, amitriptyline), and anticonvulsants (pregabalin, gabapentin) to control pain and improve sleep.
- Physical Therapy and Exercise – Aerobic and resistance training, stretching, hydrotherapy, and posture correction to enhance flexibility and reduce pain.
- Psychological and Behavioral Therapies – Cognitive Behavioral Therapy (CBT), mindfulness, and relaxation techniques for stress and anxiety control.
- Lifestyle Modifications – Maintaining regular sleep patterns, balanced diet, hydration, avoiding caffeine and nicotine, and practicing stress management.
- Complementary and Alternative Therapies – Acupuncture, massage, yoga, tai chi, and chiropractic care may provide symptom relief.
Conclusion
Fibromyalgia is a multifactorial, chronic pain condition characterized by widespread pain, fatigue, and cognitive dysfunction. Accurate diagnosis relies on clinical assessment and exclusion of other pathologies. A holistic treatment plan involving pharmacological therapy, physical rehabilitation, and psychological support can significantly enhance symptom control and daily functioning. Patient education and self-management remain essential for long-term success and improved well-being.